In order to better understand the philosophy of periodontal treatment, a brief reminder of the aetiology of periodontitis seems appropriate.
By definition, periodontitis is a pathology characterised by the appearance of a periodontal pocket.
How does this pocket form?
The infectious nature of periodontal diseases is no longer in question. The bacterial biofilm is indeed the first link in the chain. By settling in the dento-gingival sulcus, an inflammatory reaction in the marginal gingiva will ensue. Faced with this persistent and chronic irritation represented by this bacterial invasion, the immune system is powerless and, in the face of such relentlessness, will literally turn around and become a threat to the host itself.
Indeed, it is mainly the inflammatory infiltrate generated by the bacterial exacerbation that will be responsible for the successive destruction of the gingival collagen, leading to an apical migration of the epithelial attachment, and then followed by bone resorption of inflammatory origin, all of which leads to the formation of a periodontal pocket.
Periodontitis is therefore an infectious disease in which the host immune response plays a key role in the process of tissue destruction. While bacteria and their metabolites are capable of directly destroying tissue, these mechanisms are secondary to the major immune dysfunctions that the bacteria will induce.
But is this imbalance in the host-parasite balance inevitable? Is the presence of bacteria sufficient to generate this immuno-destructive reaction?
The answer is no. While the presence of bacteria is a necessary trigger, it is not a sufficient factor to induce bone resorption in all patients. In order to understand these inequalities in periodontal disease, the notion of susceptibility must be integrated. Certain factors, commonly called risk factors, will put some individuals at greater risk than others.
These elements intervene either on the bacterial parameter considered as the major etiological factor, or on the host response.
They can be divided into 4 groups:
It has been shown that of the 500 different bacterial species in the oral ecosystem, a limited number of bacterial species are responsible for the development of periodontitis (Socransky et al, 1992).
As much as there is a direct correlation between plaque accumulation and the development of gingivitis, the transition from gingivitis to periodontitis is not systematic.
Patients who neglect their oral hygiene may be at greater risk of periodontal disease, but not proportionally. However, while the presence of virulent bacteria is essential for the onset of disease, it is not sufficient to initiate it on its own. The absence of periodontal lesions in patients who are carriers of parapathogenic germs means that the host's ability to control this bacterial aggression plays an equally important role (Kornman et al, 1997).
A number of factors, this time related to the host, can disrupt the immune defence mechanisms making these patients more susceptible to periodontal infections. These factors may be innate, in other words written into the patient's genetic code, or acquired and thus secondarily induce conditions such that the periodontium will become more vulnerable to bacterial attack.
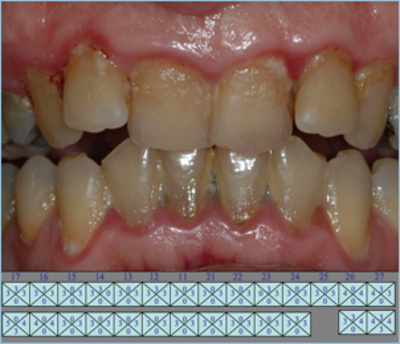
General profile:
These are the identity characteristics of the patient (age, sex, race) which cannot therefore be modified:
- Age in itself is not an etiological factor as the general public might think, but physiological tissue degradation combined with the duration of exposure to etiological factors makes it a major risk factor.
- Certain ethnic populations are more exposed to periodontal diseases and in particular to aggressive forms (Albandar, 1997).
Genetic particularities :
A genetic deficiency in a cellular component of the immune system may increase the risk of exposure to periodontitis:
- Studies of aggressive periodontitis have revealed an almost systematic abnormality of neutrophils (Page, 1985).
- The hyperinflammatory phenotype is another widespread genetic feature.
It defines a propensity to provoke an exacerbated inflammatory reaction by responding to an aggression of the same intensity with an overproduction of pro-inflammatory cytokines (PGE2, Il 1, TNF), factors which play a major role in periodontal destruction.
In addition to the non-modifiable systemic risk factors, there are a large number of modifiable factors that influence the onset and development of periodontitis to a greater or lesser extent,
depending on their "importance" and intensity.
In addition to the non-modifiable systemic risk factors, there are a large number of modifiable factors that influence the onset and course of periodontitis to a greater or lesser extent, depending on their "importance" and intensity.
Systemic diseases :
Many diseases can disturb the tissue metabolism or the functioning of the immune system and make subjects more vulnerable to periodontal bacterial aggression.
Among these, diabetes takes a particular place.
In Belgium, one person in twenty is affected. A figure that will grow exponentially over the next few years, since it is predicted that one Belgian in ten will be affected in 2020 if no measures are taken. These figures are even more appalling when you consider that one in three people are unaware of it. Why all these figures? Because we are on the front line! Many studies show that a diabetic patient is more likely to suffer from periodontal disease. Furthermore, the treatment of periodontal disease is also more difficult in a patient with poorly controlled diabetes (Taylor G., 1998). Our role is all the more important because the link between periodontitis and diabetes is thought to be reciprocal. Indeed, periodontitis would affect glycaemic control and exacerbate diabetes (Grossi S., 1998)
Tobacco:
Tobacco is recognised as a major risk factor in the development and progression of periodontal disease. The mechanism of action of tobacco is linked to its many harmful components, in particular nicotine.
The defence mechanisms against bacteria are impaired. The vascularisation of the gums is reduced, the symptoms associated with inflammation are very often masked. Smoking patients respond less favourably to periodontal treatments (especially if smoking is high).
Smoking is an element that the practitioner cannot control. It must be taken into account in the diagnosis, treatment plan and prognosis. The patient should be informed of the consequences and benefit of stopping smoking.
Medications:
The main classes that cause periodontal disturbances are: Cyclosporine (immunosuppressant), phenytoin (anti-epileptic), nifedipine (calcium channel blockers).
Many of these lesions will be increases in gingival volume or hyperplasia.
All these clinical manifestations are the result of the action of the drugs on cellular metabolism and (fat) inflammation related to the presence of plaque. They are therefore i,existing in the totally edentulous.
Stress:
Stress in relation to periodontal disease is chronic in nature and is not due to a single event. In other words, it is the inability to cope with stress rather than the stress itself that plays a role in the progression of periodontal disease (Croucher R. et al, 1997).
Stress acts on the periodontium either systemically by altering immune functions (Breivik et al, 1996), or locally. Indeed, anxious patients regularly develop compensatory parafunctions (clenching teeth, bruxism) in order to neutralise their stress. These have direct consequences on the periodontium.
All the elements that facilitate the accumulation of plaque and make its elimination by cleaning more difficult, can represent an aggression for the periodontium that it is not always ready to receive.
These retention factors include
Supra- and subgingival calculus, caries, dental malposition, defective fillings, filling overflow, overcrowding, furcation entries, fissures and defective endodontic treatments. Every imperfection, no matter how small, provides a niche for bacteria.
Iatrogenic factors, while they can harm the periodontium by promoting bacterial adhesion, can also represent a physical aggression.
Indeed, the role of the gum is above all to ensure a watertight seal for the underlying bone.
This seal is composed of a junctional epithelium and a connective attachment. It is called the biological space.
No filling material is biocompatible and would therefore allow tissue adhesion. Therefore, the boundaries of restorations cannot be made in this biological space.
A violation of this space leads to a rupture of the attachment system and chronic gingival inflammation. Tissue physiology will then wish to re-establish this balance and reform its seal under the filling, thus causing the formation of a periodontal pocket (iatrogenic in origin) which may be colonised secondarily by bacteria.
Occlusal trauma refers to excessive loads that can affect the periodontium, whether they are functional (prematurity, interference, malocclusion, reduced number of teeth), parafunctional (bruxism, lingual impulse, etc.) or iatrogenic (orthodontic treatment, removable prosthesis).
Nevertheless, occlusal trauma alone does not induce periodontal lesions. It is only an aggravating factor. Consequently, in a periodontitis context, occlusal trauma only increases bone loss and accelerates the deepening of pre-existing periodontal pockets (Ericsson I. et al, 1982).