Given the high prevalence of periodontal disease and the insidious nature of some forms of periodontitis, periodontal examination should be part of a routine examination.
Should we therefore systematically perform a complete periodontal check-up in all our patients, including a topographical map of pocket depth, plaque index and bleeding index? We don't think so, let's spare our periodontally healthy patients this tedious and burdensome examination.
Since 2006, the nomenclature has been opened to periodontology by introducing the Dutch Periodontal Screening Index (D.P.S.I). Its aim is to facilitate the screening of periodontal diseases in our daily practice.
In a few minutes, it can identify patients who require further examination and, in a second step, appropriate treatment.
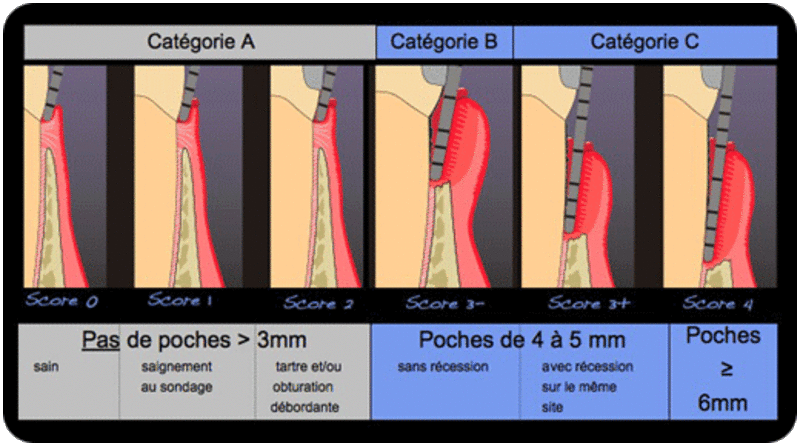
The aim of the test is to classify the patient into one of three categories A, B or C.
When the DPSI indicates that the patient requires further investigation (categories B and C), a full periodontal status will be performed.
This examination involves recording the depth of probing of all pockets, the identification of dental mobility and furcation damage. Only such an examination allows a reliable diagnosis, detailed treatment planning and, above all, a long-term evaluation of the result.
This clinical examination must be systematically accompanied by
Once we have drawn up a precise identity card of our patient's periodontal condition and before rushing to use our instruments, a diagnosis must be established.
This form of periodontitis is the most common (95% of periodontitis). It develops progressively between the ages of 30 and 40 from gingivitis. It is characterised by a chronic inflammation evolving in a slow and progressive way, by periods of activity and remission (Socransky et al, 1984). Bone loss is more often horizontal. Generally speaking, the severity of periodontal destruction is correlated to the quantity of bacterial plaque, but it may be accentuated locally by aggravating factors (unfavourable dental anatomy, dental malposition, root proximity, iatrogenic restorations, cracks, endo-periodontal lesions, etc.).
The whole dentition can be affected in a generalized way but a localized irregular distribution is more frequent (in particular on the molars).
The symptoms are as follows
This clinical entity is much rarer (5% of periodontitis).
It can also be localised or generalised (i.e. localised forms do not necessarily evolve into a generalised attack).
Aggressive periodontitis often affects young subjects. The severity of the damage correlated to the age of the patient is a diagnostic element although studies show that they can be detected at any age (Sjodin et al, 1993).
One of the main characteristics of this form of disease is that tissue destruction is not necessarily proportional to the amount of plaque or the existence of other local factors.
This brings us back to the concepts of host susceptibility and bacterial virulence factors.