If periodontitis is defined as an infectious disease, it is to be welcomed, as with all infections, that there is a treatment. This has been tried and tested for many years and is almost always successful, provided that the instructions for use are followed. There is no room for compromise when it comes to treating an infection, and the patient will not tell you otherwise. Whatever the patient, whatever their age, whatever their socio-economic status, whatever the form of their periodontal disease, aggressive or chronic, generalized or localized, severe or incipient, all periodontal treatment starts with the same box: the initial therapy. Even if each patient is different, has different requirements and needs, the same treatment protocol must always be followed.
The infectious origin of periodontitis requires daily control of the bacterial factor. The patient is therefore undoubtedly the main actor in the treatment. The key to success lies in the patient's active and lasting cooperation.
No element at the beginning (neither the age, nor the hygiene, nor the behavioural habits of the patient) allows us to prejudge this cooperation in the long term (Mendoza et al, 1991). All the patients must therefore start on the same line, and it will be enough to motivate them. Nevertheless, the task is not an easy one, as the information to be communicated to the patient is not very pleasing at first sight. We are nevertheless preparing to tell him that he suffers from an INVISIBLE, FLAMELESS disease, whose rather DESAGREABLE treatment is, moreover, not REIMBURSED by the mutual insurance company, and to finish him off, that he is condemned to come and see us regularly for the rest of his life to maintain the result obtained, in short, only good news!!!
We must have a well-trained speech to ensure this mission, and not give up. The patient is suffering from an infection, he has the right to know this. They are then free to decide whether or not to undergo treatment.
To succeed in motivating the patient, there is only one watchword: he must be valued.
How can this be done?
The principle consists in first explaining the general mechanism of periodontitis and its treatment using a deliberately technical and precise vocabulary before transposing it into the patient's mouth.
Indeed, in order to better understand what concerns him, the patient must first be given some basic notions.
To begin with, the practitioner will introduce the patient to the anatomy of the tissues surrounding the tooth, and the word periodontitis should now be as much a part of the patient's vocabulary as the word tooth. As decay, or more accurately periodontitis, is the main cause of tooth loss, it is time for the patient to update their knowledge.
We let him know that periodontitis is not a fatality that accompanies aging (contrary to popular belief), but that it is the result of bacterial aggression. In other words, it is an infection.
We then explain the process of plaque formation and inform them that plaque is the main reason for brushing (if you ask ten patients at random why they brush, none of them will spontaneously mention plaque).
Like tooth decay, the origin is bacterial, but the course of periodontal infection is much more insidious because it is painless.
The practitioner then describes successively the process of pocket formation, from gingivitis to terminal periodontitis, comparing it to a rejection reaction to a foreign body.
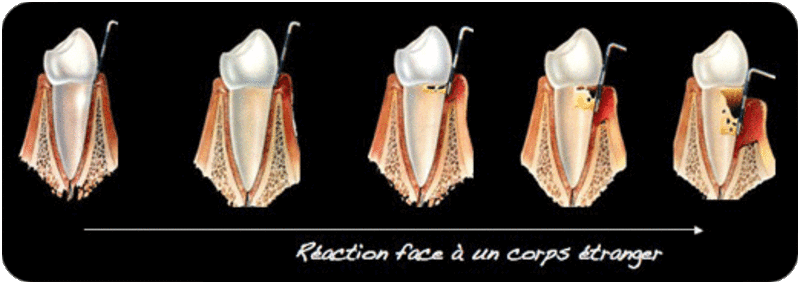
The symptoms, which are sometimes discreet and indicate the presence of inflammation, are described step by step.
At this stage, it is necessary to relieve the patient of guilt (who may become offended), by specifying that if the origin is bacterial, hygiene is not the absolute cause.
We therefore discuss the influence of general and local risk factors on the onset, evolution and treatment of the disease. This leads to profound and unjust inequalities in the face of disease.
We will focus on the factors that are most relevant to the patient. If the patient is a smoker, he or she must be aware of the harmful and insidious effects of tobacco on the periodontium and its influence on the prognosis of the disease. Let us not underestimate our role and power in getting our patients to stop smoking. On the one hand, no patient wants to lose his or her teeth inexorably and is often ready to do anything to prevent it. On the other hand, they are confronted, often for the first time, with the deleterious effects of smoking on their person.
We then continue our lesson by now addressing the general philosophy of treatment.
First of all, let us underline the importance of making a good diagnosis in order to define with precision the degree of severity of the disease and thus the treatment needs of the patient. We then give him the means to read a pocket assessment so that he can follow the evolution of his periodontal condition precisely.
In all, four rules must be assimilated to understand the logic of the treatment:
The objective of the treatment is finally presented:
To reattach the gum to the surface of the tooth in order to protect the underlying bone again. To achieve this, we will have to remove, especially mechanically, the bacteria (and tartar) that are attached to the roots and that prevent the gum from adhering to the tooth. This is called root planing.
In most cases, two sessions in close succession are sufficient to accomplish this task. However, additional local treatments (surgical or not) are sometimes necessary to perfect the result. The objective is to reduce all pockets to depths compatible with good periodontal health, i.e. less than 5 mm.
About fifteen minutes have passed since the beginning of the session. The patient is usually hanging on the practitioner's every word, waiting impatiently for the verdict. It is time to move from theory to practice. Using a mirror and a periodontal probe, we show him the existence of the gingival sulcus, the dental plaque and the associated inflammatory symptoms.
His periodontal assessment is then commented on, with emphasis on the teeth with a reserved prognosis (V. local risk factors) and we compare it with the radiographic examination.
Given the speed at which plaque forms on the surface of teeth, real-time control of this etiologic agent is the key to treatment. Hygiene may not be the absolute cause of the disease, but it is still the cornerstone of treatment. The patient is the main actor in the treatment and must be convinced of this at the end of the session. All our patients have a toothbrush and know what it is used for. What they don't know is why and, above all, how. We have answered the first question, now let's focus on the second.
Let's start by setting the scene:
Each tooth has five sides, multiply that by thirty-two and you have no less than one hundred and sixty surfaces to clean. That's how big the task is. First of all, you have to take your time: two minutes minimum.
It is clearly established that one complete daily removal of the plaque that is being organised is sufficient to prevent the onset of gingivitis.
Evening brushing (considered as medical brushing) should be preferred to morning brushing (which is more like comfort brushing), simply because self-cleaning is much less effective at night (less saliva production, less frequent swallowing, etc.).
Most studies show that using an electric toothbrush is better. However, let's put the science aside and just use a little common sense. It must be admitted that applying the modified Bass technique to the lingual surfaces of the lower molars is not for everyone. The toothbrush should be angled, without pressure, about 45° towards the gums in order to penetrate the interdental surfaces and especially to penetrate superficially into the gingival sulcus. Above all, we recommend methodical brushing, surface by surface and quadrant by quadrant, so as not to forget anything. The integrated timer in most toothbrush models is a valuable tool for distributing our work evenly.
Whatever the brushing technique, whatever the toothbrush, whatever the patient's wishes, the interdental surfaces are systematically spared by conventional brushing. The patient's periodontal assessment will often speak for itself. Two possible techniques for effectively cleaning these surfaces will therefore be suggested.
For each of them, the spirit is the same, the goal is not to clean the interdental spaces but the interdental surfaces, of which there are two per space.
The first method involves the use of interdental brushes. It has the advantage of being simple and therefore allows the patient to be immediately operational. Several brushes of different diameters are often useful, which makes the logistics a little restrictive.
The second approach concerns the use of interdental wire.
If the mastery of the brushes is generally instinctive, that of the wire is more delicate. It requires a longer and more restrictive learning phase. It is therefore necessary to be realistic and to give the patient practical advice so that the floss does not end up in the dustbin on the third day.
Its use is indicated day after day by starting, for example, with a single arch per day, giving priority to the areas at risk (generally the molar sector). In general, flossing is recommended for patients with gingivitis or mild periodontitis with narrow interdental spaces, as well as in cases of dental malposition.
Brushes, on the other hand, should be used in patients with more open interdental spaces, which are often synonymous with deeper initial lesions.
In any case, interdental cleaning is rarely part of our patients' habits to begin with.
No one will deny that there is nothing more difficult than changing habits. It is necessary to take the time to explain to the patient with a demonstration on a model, then in the mouth and finally, repeating the act in front of a mirror. The patient must understand that this is not just theoretical advice but one of the main keys to successful treatment.
Patients are often concerned about the choice of toothpaste. It should be made clear to them that the antimicrobial effect of toothpastes is of minor clinical significance. There is no substitute for careful mechanical removal.
Chlorhexidine digluconate (CHX) remains the first choice in periodontics because of its broad antibacterial spectrum (Gram +, Gram -, Candida) and its ability to bind to periodontal tissues, which gives it a more prolonged action (Addy et al, 1978). CHX is bacteriostatic and bactericidal in high concentrations. However, beware of the downside of its antiseptic properties, as the oral flora is an ecosystem that lives in balance with the host and ensures its protection, and prolonged use of CHX can disrupt this balance. Furthermore, it should be remembered that CHX only acts as an inhibitor of plaque formation but does not act on adherent plaque and therefore on the biofilm already formed (Zanatta et al, 2007). Finally, CHX used as a mouthwash has no action on the subgingival flora (Flemmig et al, 1993), so it does not act on periodontitis.
For all these reasons, the use of 0.1 to 0.2% chlorhexidine as a mouthwash is recommended, but only a few days before to a few days after a treatment (initial therapy, periodontal surgery). The aim is to massively reduce the overall bacterial load in the oral cavity during a therapeutic procedure. As for the daily use of an antimicrobial solution, some mouthwashes can be recommended as a complement to mechanical brushing, but let's make sure that the patient does not attach too much importance to the virtues of this solution as it never replaces mechanical plaque control.
A. Elimination of local bacterial retention factors
In order to optimise the benefits of our subgingival treatment, we start by eliminating (or correcting) all iatrogenic factors which, on the one hand, may prevent the patient from practising optimal plaque control and, on the other hand, may favour too rapid bacterial recolonisation.
The main factors for bacterial retention include
Indeed, supra-gingival calculus alone is not very pathogenic. Nevertheless, its rough surface provides an ideal site for bacterial adhesion.
Supra-gingival scaling will therefore often be carried out at the same time as root planing, unless it represents a major obstacle to the patient's cleaning, in which case it can be carried out beforehand.
In the first instance, damage control is achieved by polishing defective fillings and correcting overhangs directly. The aim is to achieve the smoothest possible supra- and subgingival surfaces.
B. Removal of major occlusal overloads
When an occlusal overload is found on a tooth and it locally worsens the periodontal condition (angular bone loss), an occlusal adjustment can be performed immediately. The first step is to remove the interference finely by subtraction. Comprehensive occlusal management may be necessary at a later stage.
C. Extraction of condemned teeth
The decision to extract at the outset of treatment must be based on objective, indisputable criteria. If there is the slightest doubt, it is useless to procrastinate, there will still be time to ask the question later, at the time of our re-evaluation or during the surgical treatment, on more objective anatomical criteria.
Moreover, if all the evidence is there to condemn a tooth, announcing it to the patient always remains a very delicate mission. A great deal of caution and attention must be used to gauge the patient's receptiveness to this subject.
The desired therapeutic approach is frequently in opposition to the reasoned psychological approach, which sometimes obliges us to voluntarily leave the prognosis of a tooth in doubt so as not to alter the patient's morale, which is so important for our treatment.
Deciding which tooth should be extracted from the start means knowing how to evaluate the prognosis of our treatment for each tooth.
A distinction must be made between general prognostic factors that relate to the patient and local prognostic factors that relate to the teeth.
The assessment of the patient depends on his or her systemic risk (general health), genetic risk (age/tissue destruction ratio), acquired risk (smoking), oral hygiene, but also on the patient's ability to cooperate and potential response to our treatment.
The individual prognosis of a tooth depends on its anatomical morphology (coronal and root), its location (accessibility to treatment and cleaning), its vitality, the depth of the pocket, the state of the furcation, and its mobility.
The relative influence of all these factors must be balanced with the professional experience of the practitioner. Depending on the practitioner's skills, the decision to extract one or more teeth will become apparent at an earlier or later stage of treatment.
However, the patient's ability to cooperate and, above all, his or her physiological potential to respond to our treatment must not be overlooked. These are two factors that cannot be prejudged at the outset and which therefore require the most conservative behaviour possible from the outset.
In practice, a conservative attitude is always preferred in complete dentate patients, to avoid the prejudices of a prosthetic rehabilitation. However, if a prosthetic treatment plan is envisaged, only those elements that are 100% reliable will be retained. Our absolute mission is to ensure not only good periodontal health but also the long-term sustainability of our prosthetic treatment.
D. Non-surgical root planing
Non-surgical root planing consists of removing the subgingival bacterial and tartar mass and making the root surfaces smooth and endotoxin-free in order to achieve tissue re-adhesion. In other words, the goal of the treatment is to obtain a biologically compatible root surface to allow this re-attachment.
The main component of our treatment is mechanical. It is performed with ultrasonic instruments (80% of the treatment). The insert is gently introduced blindly into the subgingival pocket, and is then pressed against the root to perform a lateral translation movement. To complete our work, we use manual curettes to obtain a smooth and clean surface.
This is a minimally invasive procedure, the soft tissue is spared as well as the cementum to avoid gingival scarring and to promote stable attachment.
The success of the surfacing procedure is based on a methodical and systematic mechanical grid that leaves nothing to chance.
Despite a significant reduction in bacterial mass, the mechanical approach is unable to eradicate all bacteria involved for three main reasons:
Antiseptics
As previously mentioned, we recommend that our patient use a Chlorhexidine digluconate mouthwash for the duration of our treatment. However, this has very little effect on the subgingival flora. Irrigation directly into the pocket is the only way to successfully deliver an antimicrobial agent in situ. This technique further reduces subgingival bacteria and delays recolonisation (Schlagenhauf et al, 1991).
Scientific studies are racing to determine the local antiseptic of first choice. It has been found that chlorhexidine (0.1-0.2%), povidone-iodine (0.5-1%) and hydrogen peroxide (1.5-3%) give comparable clinical results.
Antibiotics
Mechanical treatment combined with local antiseptics is usually sufficient to control the majority of periodontitis.
However, in the case of aggressive periodontitis, the presence of highly pathogenic bacteria justifies the use of systemic antibiotic therapy in conjunction with subgingival debridement. In addition, the presence of these bacteria in other areas of the oral cavity (jugal surfaces, tongues, tonsils) are sources of recolonisation of sites already treated by surfacing (Renvert et al, 1990).
But which antibiotic should be prescribed ?
The major periodontal pathogens with a determining responsibility in aggressive periodontitis are Actinobacillus actinomycetemcomitans (Aa) and Porphyromonas gingivalis (Pg). This list is of course far from exhaustive but is sufficient to conclude that a combination of amoxicillin and metronidazole is the best choice to reduce or even eradicate these periodontal pathogens (Winkel et al, 2001). Furthermore, we should not forget that bacteria are organised in biofilms. This formation gives them a high resistance to host defence products but also to antibacterials. Antibiotics alone therefore have no effect on periodontitis. Root planing remains the central element of our treatment.
To avoid the real risk of bacterial recolonisation from sites that have not yet been treated, we perform root planing in a maximum of two sessions, which should be as close together as possible.
The advantages of blind subgingival debridement over surgical treatment are numerous. Less traumatic, it causes less post-operative pain and especially less post-operative gingival retraction. And if surgical treatment seems unavoidable, we will always start with a non-surgical approach, on the one hand, because it allows to massively reduce the initial gingival inflammation, making the surgical procedure easier, and on the other hand, it will reduce the scope of the surgical intervention to a minimum.